Symptoms of nail infection can be uncomfortable, but most do not pose a health risk. However, if you work in a job where your hands are frequently wet, such as in the kitchen, you should talk to your healthcare provider. Waterproof gloves can help you prevent infection. Waterproof gloves also don't irritate your skin. It is important to seek treatment for paronychia if you have diabetes or have a hard time-fighting infections.
Distal subungual onychomycosis
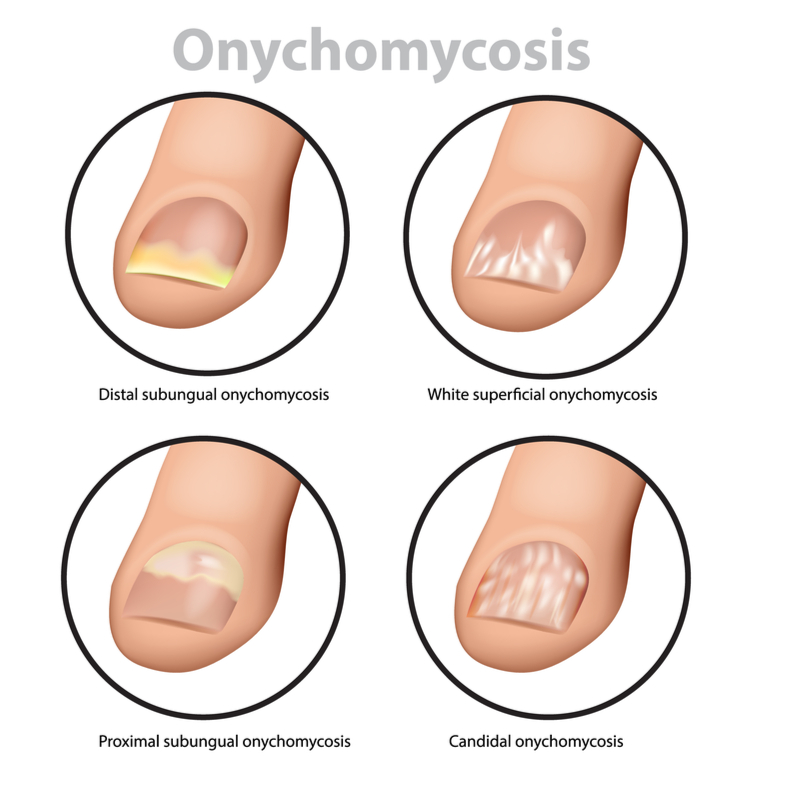
Onychomycosis is a disease that affects the nails, resulting in local pain, paresthesia, and reduced quality of life. It can affect the toenails and fingernails and is often associated with other conditions such as hyperhidrosis and tinea pedis. There are several types of this disease, and diagnosis is based on the modality of invasion.
There are several treatment options available for distal subungual onychomycoses. Among these are oral terbinafine and oral itraconazole. Itraconazole 200 mg twice a day is usually used for treatment. The success rate is around 40%, with an overall recurrence rate of ten to fifty percent. Many patients opt to avoid systemic therapy due to the potential for idiosyncratic hepatic reactions. However, in some cases, systemic therapy is the only viable option for treating this condition.
In general, the fungus growth on the nail plate is the most common type of onychomycosis. In this type of infection, the nail plate can separate, causing pain and a reduced ability to walk. Treatment for distal subungual onychomycosis is difficult and requires a professional who can accurately diagnose the underlying disease. Another type is called white superficial onychomycosis. This type of infection affects the top layer of the nail and causes a chalky appearance. It is frequently associated with the infection of the great toenail.
The diagnosis of onychomycosis is made based on a patient's history, physical examination, and diagnostic tests. Patients with this disease are likely to develop pain, social embarrassment, and impaired quality of life. Certain predisposing factors can raise clinical suspicion. Specific onychomycosis symptoms include white longitudinal streaks in the nail plate. Nonspecific clinical findings include subungual hyperkeratosis and onycholysis.
The diagnosis of onychomycosis is complicated by the fact that it is present on approximately 50% of all nails. In addition, the condition can coexist with other nail diseases. A nail unit biopsy may be necessary to make a definitive diagnosis. The disease is often difficult to diagnose and requires appropriate treatment. The first-line treatment for this condition is systemic oral therapy. In some cases, topical antifungal treatments may be used, including nail lacquer, nail gel, and nail polish.
Alcohol-based medication is a viable treatment option for this disease. Alcohol-based medications are approved by the Food and Drug Administration. These medicines include Halog Solution (halcinonide), Taclonex Scalp Solution (betamethasone dipropionate), and Clobetasol. While they may not be the most convenient treatment options, alcohol-based medications have been proven to be effective.
White superficial infections
Infections of the nail can be caused by two types of fungus: Distal subungual onychomycosis (DSON), which begins in the skin underneath the nail bed. DSON is difficult to treat and can even separate your nails. White superficial onychomycosis, however, affects only the upper layer of the nail, resulting in a white, chalky appearance. The infection is caused by a fungus that prefers warm, moist conditions.
Unlike DSO, white superficial onychomycosis is caused by certain types of fungi that cause nail decay. These fungi attack the keratin layer in the nail plate, causing the nail to become crumbly and white. While the condition may be mild, it can lead to other problems. If left untreated, WSO may spread to the deeper layers of the nail plate and cause leukonychia.
If the fungus is identified, it must be classified as a dermatophyte. However, it is not always possible to distinguish between a dermatophyte and a non dermatophyte. The latter is the most common fungus involved in onychomycosis, while the former is secondary to dermatophyte infection. The diagnosis of nondermatophyte onychomycosis is made based on the presence of atypical frond-like hyphae.
When a white superficial infection in nails is suspected, a podiatrist or foot specialist will take a nail sample for culture to determine whether it's nail fungus. The doctor may prescribe oral or topical antifungal medications to treat the condition. To treat white superficial onychomycosis, proper foot care and cleaning of shoes are key. Additionally, antifungal spray can be applied on the nail to avoid further infection.
While onychomycosis in children is not life-threatening, it is difficult to treat and may affect people with poor circulation. It can cause significant psychological stress and affect a person's daily life and occupation. Patients with this infection have lower self-esteem and suffer from embarrassment. If left untreated, it can lead to the development of more serious infections. And since treatment is difficult, the patient may become re-infected and may never recover.
While onychomycosis is contagious and spreads through direct contact and contaminated materials, it does not carry a hereditary link. Certain genes can protect against it, but it is not a risk factor in all cases. In addition, some people are more susceptible to it, particularly those with immune problems. These include people with diabetes, weakened immunity, and malnutrition. Also, older people are more likely to develop the condition.
Skin and nails are susceptible to fungal infections. Fungal infection is more common in elderly people, where aging causes nails to become brittle and dry. These nails are also susceptible to infections caused by the fungi that cause athlete's foot, jock itch, and ringworm. These fungi can also spread from one nail to another. This is a serious condition that should be treated by a doctor as soon as possible.
Treatment options
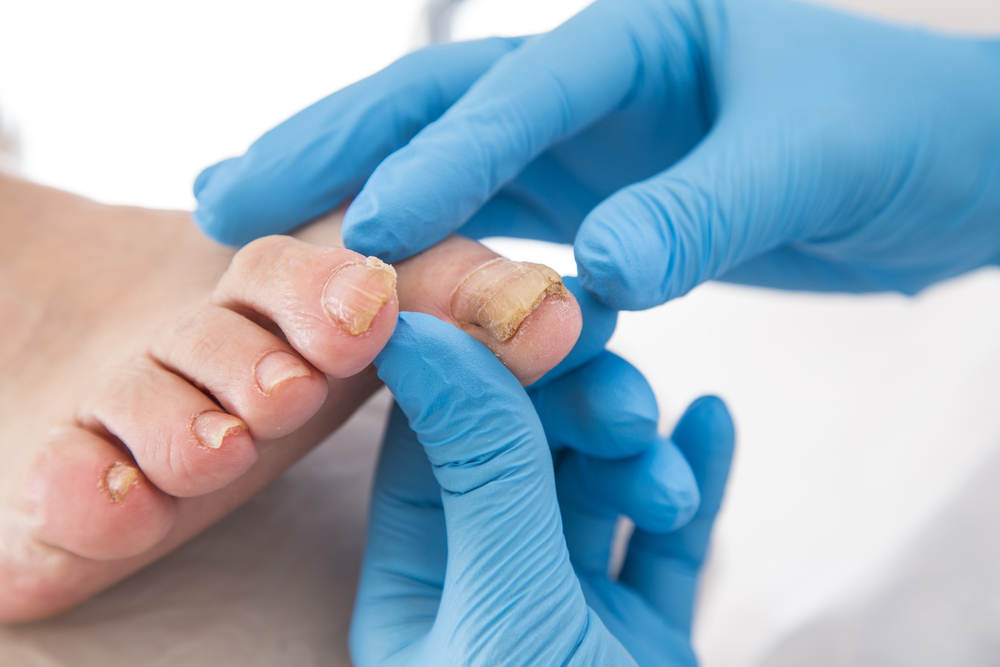
If you've noticed that your toenails are discolored, you may be wondering if there are any treatment options available. There are several treatments, ranging from oral medications to laser treatment. All of these options have their advantages and disadvantages. For example, oral medications can cause serious side effects such as liver damage or heart failure. Also, some medications require regular blood tests to monitor their effectiveness. Besides oral drugs, other treatment options include laser treatment and antifungal creams.
If you suspect that you have a nail infection, your primary care physician may prescribe antifungal pills. These medications are taken for six to 12 weeks. They can be effective for curing the infection and helping your nail grow back healthy. These medications can interact with certain medications, however, and are not usually recommended for people with liver disease. In addition, oral medications can interact with beta-blockers, so they should only be used under the supervision of a doctor.
In some cases, antifungal creams work better on thinned nails. You can also thin your nails with a urea-containing lotion or file. Some doctors may recommend the permanent removal of the infected nail if it is too thick to be treated effectively. A new, healthy nail can take as much as a year to grow. However, some fungal infections are resistant to antifungal drugs, so you may need to consider other treatment options to get rid of your infection.
Oral medications are another option for treating nail fungus. Over-the-counter topical medications can be used in mild cases but are unlikely to cure moderate to severe cases. A variety of home remedies for nail fungus are also available and can be very effective. Some people recommend using Vicks VapoRub, which contains thymol. Although it won't cure your problem, it might help you avoid a potentially harmful side effect.
Surgical removal is another option if your nail is chronically infected. Once the infection is treated, the healthy nail will start to grow back. However, it can take a long time and has risks. If you have been infected with nail fungus for a long time, you may want to consider over-the-counter treatments. These don't cost much and may clear up your infection for a while.
Laser treatment can be a useful option for treating nail fungus. It involves shining a beam of light onto the nail to destroy the fungus. However, the benefits of laser treatment are not well established. Although laser treatments have shown some success in treating nail fungi, it's not covered by most statutory health insurance companies. In most cases, laser treatment is best performed by a doctor after a diagnosis.


Leave feedback about this