The symptoms of sporotrichosis are similar to those of other fungal infections. The condition is caused by a fungus and can be transmitted by animals, including cats and armadillos. It is also possible to contract the disease by eating or inhaling sporotrichosis fungus, which can then spread to other parts of the body. It is not known how to transmit sporotrichosis from one person to another.
Table of Contents
What Is Sporotrichosis?
Sporotrichosis is a granulomatous fungal infection of the skin caused by a fungus called Sporothrix schenckii. The fungus typically infects the skin and subcutaneous tissue after being inoculated by soil or plants. While most cases occur in people ages 20-50, sporotrichosis can affect people at any age.
Infection of the skin caused by fungus sporotrichosis is common. This disease is caused by spores from the fungus Sporothrix schenckii, which is related to the mold that forms on stale bread or the yeast used to make beer. The fungus also grows on the thorns of roses and other plants, which is why gardeners are most likely to get it. However, this fungal infection can also affect dogs.
In severe cases, the disease can spread to the joints, bones, or central nervous system. If not treated promptly, the condition can progress to a more critical stage. Symptoms of this condition include weight loss, anorexia, and bone lesions. A comprehensive blood profile is essential to make a diagnosis of Sporotrichosis and a suitable treatment. You may also notice a fever and fatigue.
Sporotrichosis Symptoms
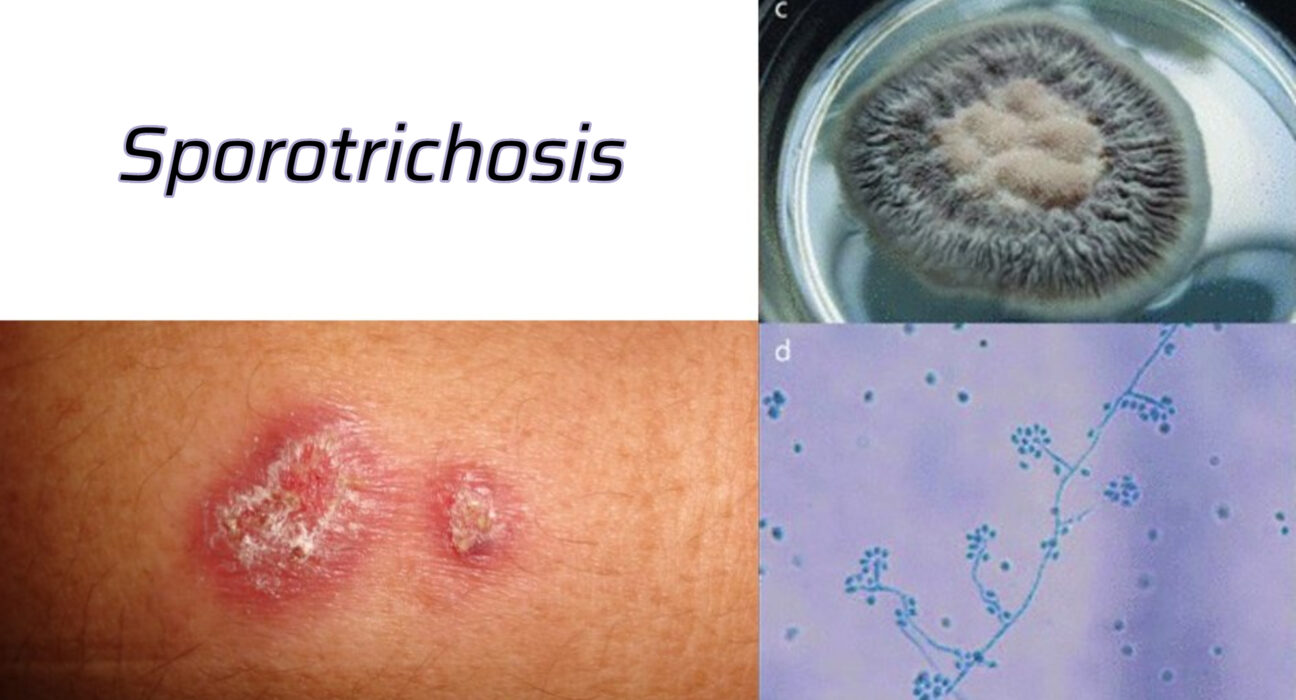
The Sporotrichosis Symptoms vary depending on the location of the infection, but the most common one is a small red bump that develops on the skin, usually on the arm or hand. The bump may develop into a sore or ulcer and may be painless or it may become red or purple, similar to an open sore. If left untreated, Sporotrichosis can progress into a more serious form and may lead to the formation of a chronic ulcer or mycetomas.
Fortunately, there are several methods of diagnosing sporotrichosis. Typically, a sample of tissue is collected and sent to a laboratory for fungal culture. Blood tests are not useful for diagnosing cutaneous sporotrichosis and should not be taken by pregnant women or those with compromised immune systems. However, in the event of severe or persistent infections, blood tests are an excellent way to confirm a diagnosis.
Treatment for Sporotrichosis depends on the site of infection and the overall health of the patient. For lesions on the skin, a solution of saturated potassium iodide is given three times a day. If oral treatments have failed, the doctor may prescribe itraconazole or fluconazole. Itraconazole is usually not effective in treating Sporotrichosis.
About Sporotrichosis
In addition to human beings, animals such as cats and armadillos can also carry the sporotrichosis fungus. The fungus can be inhaled and may infect other body parts, including the central nervous system and the brain. Although not contagious, sporotrichosis can be contracted through animal bites and scratches. Diagnosis is usually based on fungal culture.
Sporotrichosis occurs worldwide and is most common in temperate and tropical zones, where the climate is warm and humid. While large outbreaks have occurred in other parts of the world, the Sub-Himalayan region is the most common location for the disease. It is also found in the US, where approximately 200 to 250 cases occur each year. Further, it is thought to be present in ten countries in the region.
Sporotrichosis is a disease caused by a fungus known as Sporothrix schenckii. It is a fungus that inhabits dead plant material and can lead to cutaneous and extracutaneous sporotrichosis. The symptoms of sporotrichosis are often subtle and may be difficult to detect. However, if your symptoms are consistent with sporotrichosis, you should seek medical attention immediately.
How Sporotrichosis Spread
The most important thing to understand about sporotrichosis is its mechanism of transmission. The spore, a microscopic fungus, enters the body through an open wound and germinates. The spore then surfaces on the skin as a boil, ulcerating and bleeding. The sores are typically long and slender and can be painful and disfiguring. The spores can spread through the bloodstream, causing coughing and clown nose.
Sporotrichosis is not a sexually transmitted disease, but the fungus responsible for causing it is dimorphic. It can take the form of a yeast-like form, or a hypha-producing one. The fungal organisms can enter the body through skin punctures, and the fungus is inhaled. In immunocompromised hosts, the fungus can spread to other organs. It can also develop as an isolated occurrence in a person. Although there is no proof that Sporotrichosis is contagious, it can be spread through animal bites, scratches, or wounds. Symptoms of sporotrichosis are non-specific and may be difficult to detect, so it is best to be checked by a doctor.
The infection starts with a small, red, or purple bump, usually on the skin. This bump will eventually turn into an ulcer and may enlarge to a larger size. It may take several months for the first symptoms to appear, but it can last for years. The disease can also lead to pneumonia and can affect the bones and the nervous system. Although it is rare, it can lead to serious complications if untreated.
Sporotrichosis Diagnosis
The Diagnosis of Sporotrichosis can be tricky. The disease presents with pink to purple patches and may be indistinguishable from other pulmonary conditions. This is why the disease often goes undiagnosed. In many cases, the disease is not detected until it has progressed to a more severe stage. To get a correct diagnosis, it is important to consult a physician or dermatologist.
Typically, sporotrichosis is diagnosed by performing a biopsy on a skin lesion. Other diagnostic techniques may include cultures of sputum or blood samples. If sporotrichosis has spread to other body parts, blood cultures are necessary to determine whether the infection is widespread. In severe cases, blood tests may be necessary to confirm the diagnosis, but can't be performed on cutaneous lesions.
Symptoms of sporotrichosis include a pink, red, or purple bump on the arm or hand. The bump may become sore or ulcerated. It can also be contracted through a bite from an infected animal. The symptoms of sporotrichosis are similar to those of a cold or the flu. During the infection, it can also affect the eyes, causing conjunctivitis.
Sporotrichosis Treatments
While there are no effective home remedies for sporotrichosis, there are many medical procedures that can alleviate the symptoms and treat the disease. Although sporotrichosis is generally not life-threatening, open ulcers may become infected with bacteria and lead to secondary infections. If you notice a rapidly growing ulcer on your skin, seek medical attention right away. Sporotrichosis can be diagnosed by culture of a fungus isolated from the lesions and identification with fluorescent antibodies.
Topical treatments for cutaneous sporotrichosis include a saturated solution of potassium iodide and itraconazole. SSKI and terbinafine should not be used during pregnancy or lactation. Infection-causing sporotrichosis in infants requires consultation with an infectious disease specialist. Alternative treatments for cutaneous sporotrichosis are sometimes mentioned in lay literature. Fungicidal herbs can be applied directly to infected skin to kill sporotrichosis fungus. However, there is no clinical research to support this practice, and repeated visits may be required to monitor its effectiveness.
The fungus responsible for sporotrichosis lives in sphagnum moss, hay, and soil. It can be inhaled and cause pulmonary infections. Luckily, this infection is not transmitted from person to person. It can be acquired from a bite or scratch from an infected animal. Fungal culture can be used to diagnose sporotrichosis. However, serological tests do not always work.
Risk & Prevention for Sporotrichosis
If you have ever handled roses, you may have heard of the disease, known as sporotrichosis. It is caused by fungi found on rose thorns, soil, and moss. The thorns force the spores under the skin and can be contracted through contact with soil and hay. In some cases, animals bite the infected person, resulting in a pneumonia-like illness.
In animals, the fungus causing sporotrichosis is easily transmitted. Infected animals may scratch humans, and the spores can be breathed in by a human. Infected animals may also infect parts of the body other than the skin. Although the disease is not contagious among humans, cats can spread it to other parts of the body. The first symptom of sporotrichosis is a firm bump that can develop into an open sore and chronic ulcer.
A healthcare provider may recommend a course of antibiotics for a short period of time. However, some infections can last for months or years, so prevention is the key. It is important to seek medical treatment for sporotrichosis as early as possible and make sure you get regular examinations to monitor your health and avoid serious infections. The disease is often asymptomatic, and the best course of treatment is to undergo periodic antifungal medicines. The most common antifungal medications for skin sporotrichosis are itraconazole, ketoconazole, and supersaturated potassium iodide.

Leave feedback about this