The symptoms of onychomycosis can be painful, irritating, and socially embarrassing. In severe cases, the condition may even result in inflammation and pain in the affected area. Visual examination of the nails can make the diagnosis. Because there are several causes of the symptoms, it is important to perform a differential diagnosis before deciding on treatment. If a patient experiences any of these symptoms, he or she should see a doctor.
Table of Contents
Distal subungual onychomycosis
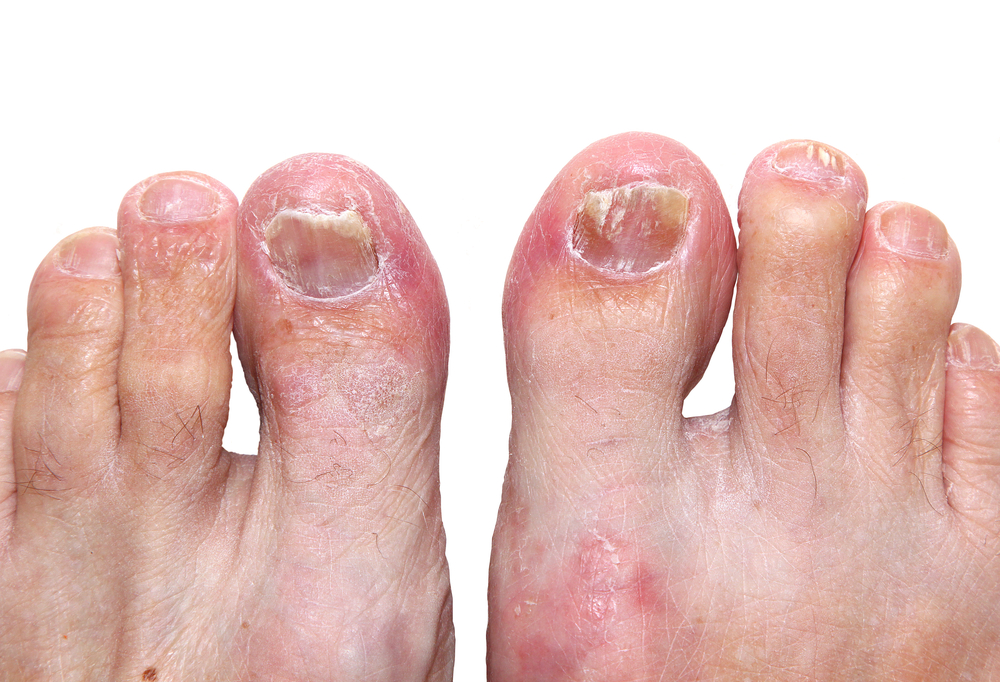
This type of onychomycosis may be diagnosed by histopathological examination and histological tests. The culture of filamentous fungi was the gold standard of diagnosis. The test was positive in 34.4% of patients, but sensitivity and specificity were low. The condition can also be recurrent, making it important to find a cure quickly. Patients with this type of onychomycosis may be at risk of developing recurrent infections of their toes.
The most effective treatment for severe forms of onychomycosis is an oral therapy, but this therapy is not appropriate for everyone. Furthermore, many patients would prefer a topical treatment. In this regard, there are numerous over-the-counter and prescription products that can be used. Various FDA-approved topical treatments for this condition have also improved the complete cure rate. Among them, the tavaborole solution has a nine percent cure rate for mild-to-moderate cases of distal subungual onychomycosis.
This condition causes local pain and paresthesia and can greatly limit the quality of life. It affects both fingernails and toenails and can be associated with other conditions, such as psoriasis and hyperhidrosis. Onychomycosis can be treated with oral terbinafine and itraconazole. It is estimated that approximately 10% of the population has distal subungual onychomycosis.
Treatment for onychomycosis depends on the modality of nail invasion, fungus species, and a number of affected nails. Because this condition is extremely deep-seated, drug treatments can't reach all affected sites. In cases where DSO has spread more than 50% of the nail, systemic oral therapy is recommended. Topical antifungals can be delivered in the form of a gel, cream, or nail lacquer.
Treatment with alcohol-based medications is a viable option for this condition. In most cases, these medications are FDA-approved and have minimal side effects. The treatment usually takes from one to three months before a positive response is noted. In some cases, the affected nail bed will return to normal and the nail plate will be reattached to it. This method is also easy to obtain. Unlike systemic antifungals, alcohol-based topicals can target fungus without the need for painful injections.
Suppurative white onychomycosis
Suppurative white onychomycosis is an infection of the toenails caused by a fungus. It results in white patches on the nail plate and mainly affects immunocompromised individuals and children with thin toe plates. Other forms of onychomycosis involve the proximal and subungual nail plate and often involve infection of the nail unit through the cuticle. Paronychia may be a sign of a bacterial infection such as Candida.
Suppurative white onychomycosis can be a difficult condition to diagnose, despite its prevalence. The fungi that cause the infection vary in their mode of development. The majority of cases of superficial white onychomycosis are caused by T. mentagrophytes, a species of dermatophyte mold that can be cultured. Less common causes of this infection include yeasts, non dermatophytes, and Acremonium. Fusarium is only found in less than 10% of cases.
In addition to a variety of fungi, suppurative white onychomycoses may be caused by mixed infections of dermatophytes, molds, and yeasts. Some other causes of onychomycosis include trauma, immobilization, and a condition called chronic venous insufficiency. HIV infection can also reduce the body's immune defenses.
Suppurative white onychomycosis is a common nail disease with significant psychological and physical morbidity. The increased prevalence of comorbid illnesses and HIV have contributed to the increased incidence of the disease. The most common etiologic agents include Non-dermatophytic molds and Candida species. However, if you have a history of trauma, a doctor should suspect an NDM infection as the cause.
Dermatophytosis
Dermatophytosis and onychomycosis are common fungal infections of the skin and nails. These infections are caused by organisms called dermatophytes, which are fungi from three genera. Dermatophytes are classified according to the mode of transmission, with zoophilic dermatophytes infecting animals, geophilic fungi infecting humans, and anthropophilic fungi affecting human skin. Listed below are some of the most common dermatophytes and the diseases they cause.
Dermatophytes and onychomycosis can be caused by a variety of fungi, including molds and Candida species. These conditions may be aggravated by occlusive footwear or repeated trauma to the nails. In some cases, a concurrent disease, such as a respiratory infection or immunodeficiency, may cause the infection. The treatment for these conditions is highly variable.
Nonprescription antifungals have been studied for onychomycosis treatment in small studies. In one study, 18 patients with onychomycosis were treated with topical mentholated ointment for 48 weeks. The disease resolved in 28% of the patients, while 56% achieved partial or complete clearance. A few studies have also evaluated the effectiveness of snakeroot extract, which comes from the sunflower family.
PSO is most commonly caused by T. rubrum and affects fingernails more than toenails. Infected nails become thick and discolored and may exhibit varying degrees of onycholysis. The nail plate is not affected in the early stages, and the infection may be confined to one side of the nail, or it may spread to the entire nail bed.
Treatment with systemic drugs for onychomycosis is costly. Toenail onychomycosis usually requires a long course of treatment. The duration of therapy is also increased in the context of immunosuppression. However, the cost-benefit ratio of systemic antifungal therapy for onychomycosis can be evaluated according to the patient's risk-benefit ratio.
Efinaconazole 10% solution is an effective topical treatment for subungual onychomycosis. The newer, triazole antifungal treatment was approved in June 2014 by the FDA. This new treatment option is a topical solution that does not require the debridement of the nail and is well tolerated by patients. The results indicate a positive impact on patient satisfaction and QOL.
Treatment
Currently, treatment of onychomycosis requires several approaches. The gold standard is a culture test, although PCR is increasingly used. Both oral and topical treatments are generally recommended. Combination therapies and device-based treatments may improve the cure rates. Further study is needed to determine which treatments are most effective. However, new antifungal agents are available for onychomycosis.
Oral antifungal medications are the most common treatment options for onychomycosis. Oral antifungal agents such as ketoconazole, ciclopirox, and itraconazole are also available. These medications require lengthy treatment, however, and they have a high relapse rate. The adverse side effects of oral antifungal agents include an increased risk of hepatotoxicity.
A recent study published in the J Am Acad Dermatol Journal identified two novel antifungal strategies for onychomycosis. In the same journal, Gupta AK and Hay RJ described non dermatophyte mold onychomycosis and proposed a revision of the clinical classification. These findings are promising for improving patient care. For more information, see:
If you have a mild case of onychomycosis, oral antifungal agents may be prescribed. In addition to oral antifungal agents, topical creams or topical solutions may also be recommended. These treatments have limited success in controlling the disease, however, but they are often effective. However, they are still insufficient in some cases. Moreover, the side effects can be severe.
Another treatment option is the use of a number-15 blade to scrape off the infected debris. This method also removes the healthy nail plate. Then, a sharp curette is used to scrape away the material in the infected nail bed. The infected material should be collected at the proximal and lateral edges of the nail. If this treatment fails, repeat the procedure until the condition clears up.
Besides oral antifungal agents, the right toenail should be examined carefully. A 31-year-old Japanese woman presented with a whitish toenail. Before consulting the dermatologist, she had been taking topical terbinafine for two years. Due to her advanced age, oral antifungal agents were no longer prescribed. The physical examination revealed subungual hyperkeratosis, yellowish discoloration, and onycholysis in the distal portion of her left great toenail. Microscopic examination revealed branching hyphae. The diagnosis was made.