Yellow toenails are not a fun situation to have, and they are not easy to get rid of. It may take a little time to correct, and at-home treatments may not do the trick. If you're experiencing these symptoms, you might want to consult a podiatrist. This professional can help you determine what's wrong and make the necessary treatment. There are several reasons why yellow toenails can occur, including aging or infection.
Table of Contents
Onychomycosis causes yellow toenails
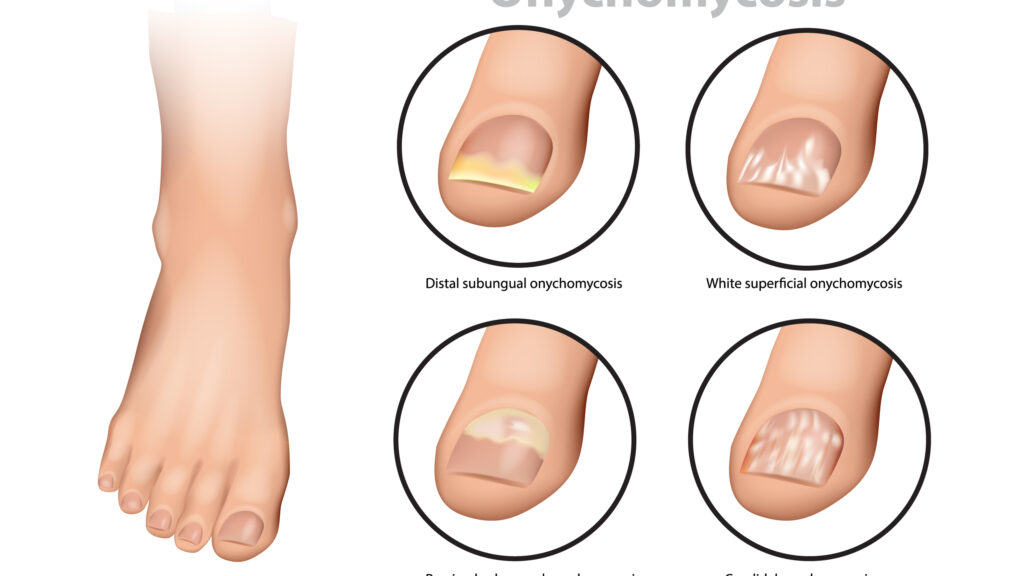
Fungal infection of the nail caused by dermatophytes can cause yellow toenails. They grow on the keratin that makes up the skin and nail. About ten percent of the adult population is prone to this condition. As we age, the likelihood of developing this disease increases. People over 70 years old are twice as likely to contract the disease as younger adults. Additionally, people who are prone to poor circulation are at greater risk of developing this disorder.
There are several possible causes of yellow toenails. Excessive use of nail polish or fungus can cause the yellowing of toenails. Other symptoms of the infection include nail thickening, splitting, or indentations. The most common cause of yellow toenails is a fungal infection. It usually affects men more than women, and is contracted through public places. It is possible to contract the infection from a skin disease known as athlete's foot, which can spread to the nails.
If the fungus is present under the nail, it is referred to as proximal subungual onychomycosis. The infection affects the part of the nail closest to the base of the toe. When this happens, the nail may be discoloured or brittle. The skin underneath the nail may also become inflamed or painful. Some people experience white spots on the nail bed, scaly skin next to the nail, and a foul smell. Because of its appearance, onychomycosis can lead to psychological problems for people who suffer from it.
The most common risk factors for onychomycosis include diminished blood circulation and prolonged exposure to fungi. Additionally, nails that grow slower than normal are more susceptible to infection. This type of infection can be difficult to differentiate from other common conditions, such as psoriasis and trauma. Moreover, onychomycosis is difficult to differentiate from psoriasis and other fungal infections, so physicians usually culture nail debris and culture it for fungus growth. Then, the diagnosis can be confirmed and the appropriate treatment can be initiated. However, the average cure rate for onychomycosis remains low.
Aging causes yellow toenails
If you've always wondered what causes yellow toenails, you're not alone. Many people don't realize that their nails are a window into their overall health. Discoloration, lifted or discolored nails can be symptoms of several diseases. While yellowing nails themselves are not dangerous, they might be signs of a more serious condition, such as fungus or infection. It's important to know the causes of your yellow toenails, since some causes are less than pleasant.
A fungus or overuse of nail polish are two common causes of yellow toenails. Stopping the overuse of nail polish will help you get back your natural nail color. Antifungal medications can help treat fungal infections, and some of them last for up to a year. To get your feet and nails back to their natural color, you may have to go to a podiatrist to get them trimmed or treated.
Symptoms of yellow toenails are a sign of a more serious condition. This syndrome affects the lymphatic and respiratory systems, and typically affects people in their 50s. In some cases, yellow toenails can be an indicator of a more serious problem, such as cancer or lymphedema. Treatment involves compression and topical and oral vitamin E. Self-tanning may also contribute to yellow toenails, but you must make sure to wear gloves while applying it.
Fungal infections are caused by dermatophytes that live on keratin, the substance that makes your nails and skin strong. About 10 percent of adults develop onychomycosis, a fungus affecting the nails and skin. The risk of getting fungal infections increases with age, as it affects half of the population over the age of 70. As age increases, so does the risk of foot disorders.
Psoriasis causes reddish nails
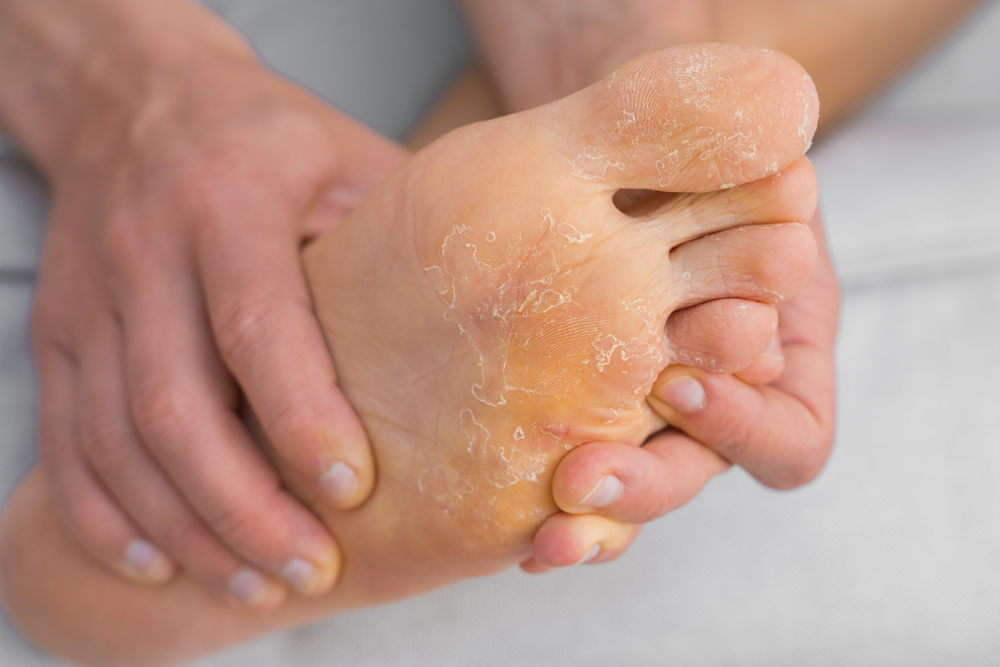
Psoriasis causes reddished nails. The condition usually begins as a small white spot and may eventually spread to the cuticle. Other symptoms include pitting, Beau lines, and splinter hemorrhages. In severe cases, the nail may crumble. Psoriasis may also cause nail fungus and inflammation. Here are some of the most common symptoms.
When a patient has psoriasis, new skin cells grow every three to four days. This process can lead to thick, reddish patches on the skin and joints. It also affects the nails, though they are not as prominent as the skin. Patients suffering from this disease also experience a rash on their skin. Fortunately, the condition is not contagious. A physical examination by a healthcare provider can help identify psoriasis. The healthcare provider will examine the affected areas, ask about symptoms, and gather family history.
Although nail psoriasis can be difficult to detect, cosmetic solutions are available that help patients disguise the condition. Artificial nails may seem attractive, but they contain chemicals and can damage the nail bed. Psoriasis patients should avoid wearing artificial nails and soaking their hands in warm water to remove buildup. Keeping nails short helps keep them clean and prevent breakage. You should also avoid prodding or removing your cuticles.
In some cases, fungal infections may cause nail thickening. In addition, some treatments for these fungal infections can exacerbate the condition. Other causes include trauma to the nail bed such as pressure from shoes, cold sore virus, and some medications. Psoriasis causes reddish nails in both the ventral and dorsal folds of the nail. In severe cases, nails can separate from the nail bed, which is the skin beneath the nail plate.
Onychomycosis causes pitting of the nails
Onychomycosis, or fungal nail infection, is a common and often serious disease with a high prevalence in the United States. It is associated with significant morbidity and can interfere with a person's social and work lives. The disease is caused by various molds that are not dermatophytes. Diagnosis requires direct microscopy, and the differential diagnosis may include psoriasis, lichen planus, or nail trauma.
The basic anatomy of a human nail includes the lunula, nail plate, matrix, and eponychium. A microscopic fungus may invade the nail plate, causing a fungal infection called onychomycosis. This condition also leads to white marks on the nearby nail. If not treated, the condition can lead to leukonychia.
Molecular testing for the diagnosis of onychomycosis has improved greatly in the last decade. Several fungi have been implicated in onychomycosis, although the most common culprit is the yeast C. albicans. Nondermatophytic fungi such as Alternaria, Aspergillus, and Acremonium can also invade the nail unit directly.
Current therapies for onychomycosis aren't effective in curing the disease. One in five patients isn't cured with griseofulvin. Some patients may need to take longer to reach a full cure than others. In addition, treatment may be complicated by slow nail growth or drug-resistant microorganisms. For this reason, the disease is considered a chronic condition.
Pitting of the nails is a common sign of onychomycosis, although it is not specific enough to diagnose the disease. Nail psoriasis may also occur in the external ear canal or on the scalp. The fungus may invade the free edge, sulci, or damaged cuticles. It may affect toenails more than fingernails.
Onychomycosis causes pain
Onychomycosis, or fungal nail infection, affects both fingernails and toenails. It is caused by a variety of fungi and can affect both nail plates and the nail bed. The symptoms of onychomycosis include pain and discomfort, nail deformity and discoloration, and a foul odor. In extreme cases, it can cause permanent damage to the nails and even reduce a person's quality of life.
In addition, to treat the problem, patients must clean their nails with alcohol before seeing a doctor. A sample of the nail bed should be obtained from the area closest to the cuticle and lunula. In addition, the surface of the nail can be removed and examined if it shows signs of superficial onychomycosis. If the infection is not accompanied by these symptoms, subclinical onychomycosis should be suspected.
Yellow toenails may be a natural occurrence of aging. As a person ages, their nails naturally change in color, thickness, and shape. However, some people are more susceptible to the yellowing of their toenails than others, and may experience pain when walking. To prevent yellow toenails, people must practice good foot hygiene. Yellow toenails can also be a sign of an underlying medical condition.
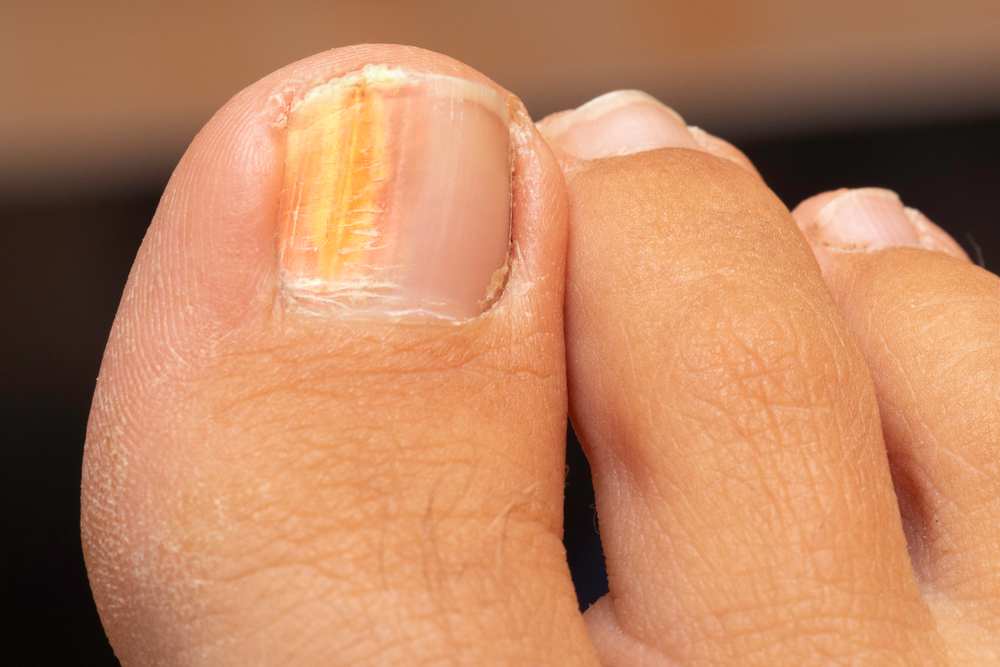
Typically, oral medication will cure onychomycosis, but it may have side effects. Oral medications for fungal nail infection may result in diarrhea, headaches, and decreased sense of taste. The most common oral antimycotic drugs for the condition are itraconazole and terbinafine. However, these two treatments are not recommended for individuals with certain medical conditions, such as liver failure, or those with poor heart function.

Leave feedback about this